Epidermolysis Bullosa or Ampollosa: Causes and Effects
Epidermolysis Bullosa is a rare disease of the skin that causes fragility and blisters. Learn how to treat it.
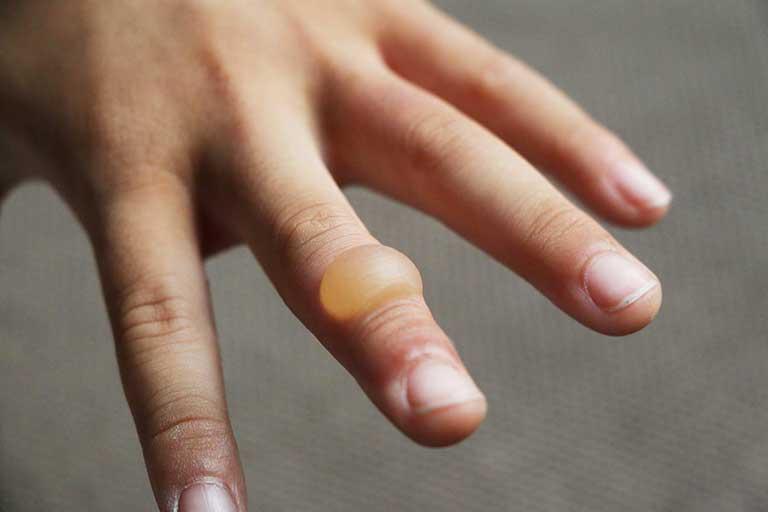
What is epidermolysis bullosa?
Epidermolysis bullosa or ampollosa - also called the “butterfly skin disease” - is a group of rare diseases that cause fragile, blistering skin. The blisters may appear in these patients in response to a minor injury, even from heat, rubbing, scratching or adhesive tape. In severe cases, the blisters may occur inside the body, such as the lining of the mouth or the stomach.
Most types of epidermolysis bullosa are inherited. The condition usually shows up in infancy or early childhood. Some people don't develop signs and symptoms until adolescence or early adulthood.
Currently, between 15 and 19 per one million subjects are born with this condition, with an estimated incidence of 10 affected subjects per one million people.
What causes epidermolysis bullosa?
Epidermolysis bullosa is usually inherited. The disease gene may be passed on from one parent who has the disease (autosomal dominant inheritance), or it may be passed on from both parents (autosomal recessive inheritance) or arise as a new mutation in the affected person that can be passed on.
The skin is made up of an outer layer (epidermis) and an underlying layer (dermis). The area where the layers meet is called the basement membrane. The various types of epidermolysis bullosa are largely defined by which layer the blisters form in.
How to detect epidermolysis bullosa?
Patients with epidermolysis bullosa have fragile skin that blisters very easily. At the slightest trauma, lesions occur in the form of blisters that scarify when they heal, i.e. they form scars. These are usually very prominent and complex and may entail retraction of the surrounding skin. Blisters or lesions may appear all over the body, on the outer layer of the skin, but also in the mucosas, such as the mouth, the nose, the eyes, etc.
In the most severe versions of the disease, scarred lesions may reduce the size of the mouth, limit the opening of the eyes, or even join fingers or toes together. Internal lesions may also occur, such as in the esophagus, preventing a proper diet and therefore leading to the patient's malnutrition. This type of scar must be clinically treated to be stabilized and/or reduced as much as possible.
On the contrary, patients with less severe variants usually suffer localized blisters mainly on hands, feet, knees and elbows or the trunk, and usually without the extreme scarring observed in more severe cases. Dystrophic nails, particularly toenails, are common and usually the most obvious manifestations in these cases.
A doctor may suspect epidermolysis bullosa from the appearance of the affected skin. Some laboratory tests may be needed to confirm the diagnosis, that may include skin biopsy, or genetic test.
How to prevent epidermolysis bullosa?
It's not possible to prevent epidermolysis bullosa, but some actions can be taken to prevent blisters and infections.
- Handle your child gently.
- Take special care with the diaper area.
- Keep the home environment cool.
- Keep the skin moist.
- Dress your child in soft clothes.
- Prevent scratching.
- As your child grows, encourage him or her to be involved in activities that don't cause skin injury. Swimming is a good option. For children with mild forms of epidermolysis bullosa, they can protect their skin by wearing long pants and sleeves for outdoor activities.
A C-section birth is recommended in those cases where the diagnosis is previously known.
How to treat epidermolysis bullosa?
This chronic disease does not have a treatment, but it is important to treat its symptoms (blisters and lesions). Blisters must be drained and covered with padded, non-adherent materials, usually wrapped in elastic bandages. In most severe cases, it is important to monitor patients' malnutrition and growth and, if necessary, supplement or modify their diet.
Due to these patients' increased risk of developing squamous cell carcinoma, it is important to monitor abnormal-looking lesions that don't heal or have abundant scar tissue, especially after age 20. Furthermore, it is recommended to conduct annual ECGs to identify heart conditions, and bone mineral density studies to identify osteoporosis.
Bibliography
- Debra Org. EB in Depth. 2020 January [Revised 2020 March]. Available at: https://www.debra.org/about-eb/eb-depth
- Mayo Clinic. Epidermolysis Bullosa. 2018 March [Revised 2020 March]. Available at: https://www.mayoclinic.org/diseases-conditions/epidermolysis-bullosa/symptoms-causes/syc-20361062
- Medline Plus. Epidermolysis Bullosa. 2018 October [Revised 2020 March]. Available at: https://medlineplus.gov/ency/article/001457.htm
- Fine, JD, JAMA Dermatol. Epidemiology of Inherited Epidermolysis Bullosa Based on Incidence and Prevalence Estimates from the National Epidermolysis Bullosa Registry. NCBI [Internet]. 2016 November [Revised 2020 March]. 152(11):1231-1238. Available at: https://www.ncbi.nlm.nih.gov/pubmed/27463098. doi:10.1001/jamadermatol.2016.2473.

