All about Psoriasis
Psoriasis is a chronic skin disease that causes red, scaly plaques anywhere on the body. It can decrease the quality of life, but there are effective treatments to control it.

What is Psoriasis?
Everything you should know
Psoriasis is a chronic inflammatory disease that involves the skin and nails, and it is associated with a number of comorbidities.
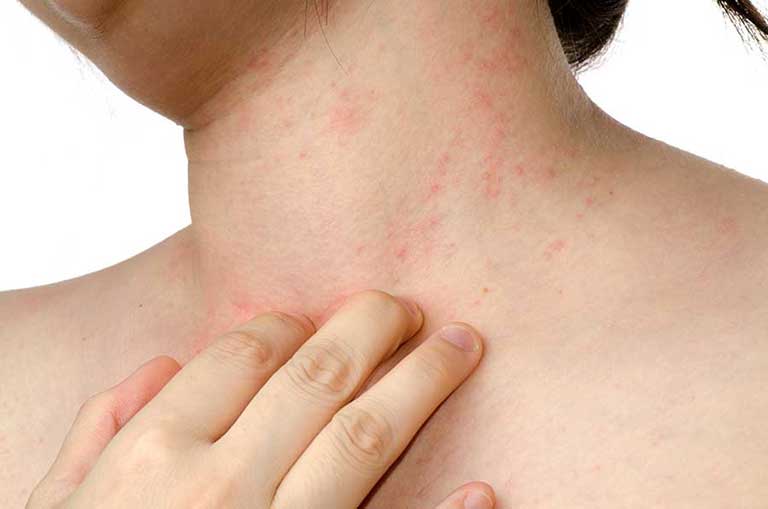
The inflammation manifests in the skin as localized or generalized patches. These patches can be red, (on Caucasian skin) or dark (on darker skin tones) flaky, itchy and scaly.
Chronic psoriasis is a lifelong illness. The periods in which the plaques occur are called flareups and the periods in which they disappear are called remissions. The disappearance of patches does not necessarily mean that the psoriasis is cured, since this resolution is only temporary. Flare-ups and remissions are part of the normal clinical course of psoriasis.
The inflammation from psoriasis can affect the nails (nail psoriasis), as well as joints and tendon insertions (known as psoriasis arthritis).
In addition, people with psoriasis are more likely to suffer from other chronic diseases, such as diabetes and cardiovascular disease, reason why early detection and proper treatment of these diseases by the doctor is of outmost importance to prevent their progression.
Psoriasis causes great physical, emotional and social burden, affecting daily life. Additionally, social exclusion, discrimination and stigma have a high impact on the person suffering from psoriasis and their families.
Psoriasis is universal in occurrence. Psoriasis may begin at any age, but it is uncommon before the age of 10 years. It is most likely to appear between the ages of 15 and 30 years. In adults, the prevalence of psoriasis varies between 0.17% in East Asia to 2.5% in Western Europe. Psoriasis appears to be equally common in males and females. An estimated 60 million people have psoriasis worldwide.
Psoriasis is not contagious. Psoriasis lesions are not infectious.
What causes psoriasis?
The exact cause of psoriasis is unknown, although there is evidence for genetic predisposition. Possession of certain human leukocyte antigen (HLA) class I antigens, particularly HLA-Cw6, is associated with an earlier age of onset and with a positive family history.
Psoriasis can also be provoked by external and internal triggers, including mild trauma, sunburn, infections, systemic drugs and stress.

Role of the immune system in the development of psoriasis
The function of the immune system is to defend ourselves against infections and other external aggressions. In psoriasis, the immune system is activated in an unbalanced manner. As a result, the skin's cell turnover cycle is accelerated. Normally, some of these cells, the keratinocytes, undergo a renewal process (that is, they die and are replaced by new cells) about every 28 days. In people with psoriasis, the renewal cycle is about 10 times faster. This causes the keratinocytes to build up and form red raised patches or thickened plaques covered with scales.
How to detect Psoriasis?
The presentation of plaque psoriasis, the most common type of psoriasis, is quite typical, and hence the doctor will most likely suspect that diagnosis just by examining your skin. However, when the lesions are not typical or in case of doubt, a skin sample is taken and analyzed (biopsy) to confirm it is in fact psoriasis.
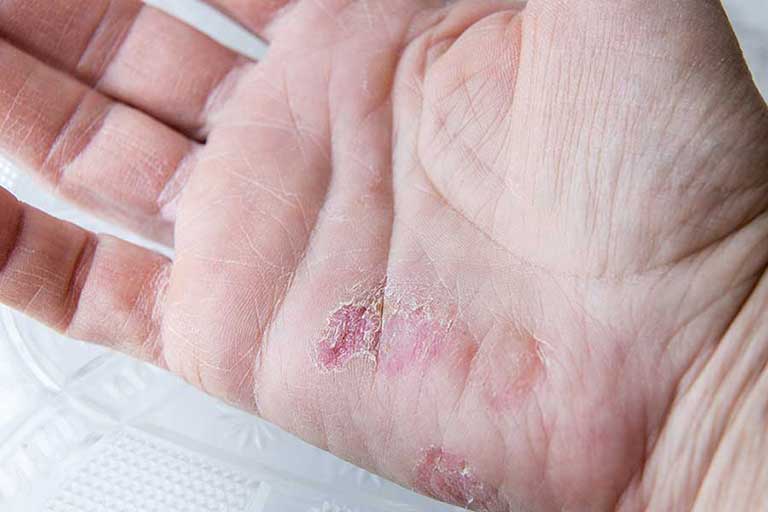
Plaque psoriasis 9 out of 10 people with psoriasis have this type6 of psoriasis. It is characterized by areas of raised, reddish skin with whitish or silver scales. Their size is variable ranging from small patches to large plaques that can cover a large body surface. They are often itchy and painful, and they can crack and bleed.
Psoriasis can occur in any part of the body, with the most typical locations being the elbows, knees, scalp and the lower back. Psoriasis is commonly symmetric, that is, if it develops in one elbow it will also appear on the other. Other areas that can be affected are the nails, folds, palms of the hand and soles. In fact, as discussed above, psoriasis can develop in any area of the skin, even in the mucous membranes (for instance, inside the mouth).
Other types of psoriasis
Besides plaque psoriasis, there are other types of psoriasis:
- Psoriasis guttate or drop-shaped psoriasis. It is the most frequent form in children and adolescence. It is characterized by reddish, drop-like papules (hence the name) and plaques, mainly involving the trunk, arms and legs, although it can affect any part of the skin. The onset of this type is associated with streptococcal infection of the upper respiratory tract and prior skin symptoms. They typically occur following an infection, usually involving the throat.
- Pustular psoriasis. This type of psoriasis manifests as pustules (blisters of noninfectious fluid) that can involve either small areas such as palms of the hands or the entire body surface.
- Erythrodermic psoriasis. It is the most serious type of psoriasis, although it is very rare. It can cause severe itching and pain, all or nearly the entire skin turns red, flakes off and falls off as sheets. In addition, there is fever and poor general condition.
Psoriasis and other diseases
Psoriasis can be associated with other diseases. It is believed that 7 out of 10 people with psoriasis have, at least, one other related disease (known as comorbidities).
Some of the diseases that can be associated to psoriasis include psoriatic arthritis, diabetes, cardiovascular diseases (such as myocardial infarction or angina), hypertension, dyslipidemia, and fatty liver.
A correlation has also been found between psoriasis and several autoimmune diseases: alopecia areata, celiac disease, systemic sclerosis, Crohn's disease, ulcerative colitis and vitiligo.
Psoriasis severity
To assess the severity of psoriasis, there are a number of indexes which take into account different aspects of the disease. One of the most widely used index by dermatologists is the PASI score (Psoriasis Area and Severity Index), which assesses the intensity and extension of psoriasis plaques. Having small plaques on the elbows is not the same as having many large itching plaques. Based on the findings, the doctor will classify psoriasis as mild or moderate to severe. This will help the clinician determine the most appropriate course of treatment in each case.
Impact on Quality of Life
Moreover, how you specifically cope and live with the condition, is also important when evaluating your psoriasis. If psoriasis affects visible body areas and you work facing the public, you may feel that your psoriasis is significantly affecting your quality of life. On the other hand, someone covered up at their workplace may not be so concerned. No one knows better than you how the disease is affecting your life.
Can psoriasis be prevented?
Psoriasis cannot be prevented. However, several triggering factors have been identified (i.e obesity, tobacco smoking, certain infections as tonsillitis or periodontitis, stress). Understanding and minimizing these triggers can be an important part of managing psoriasis.
How is psoriasis treated?
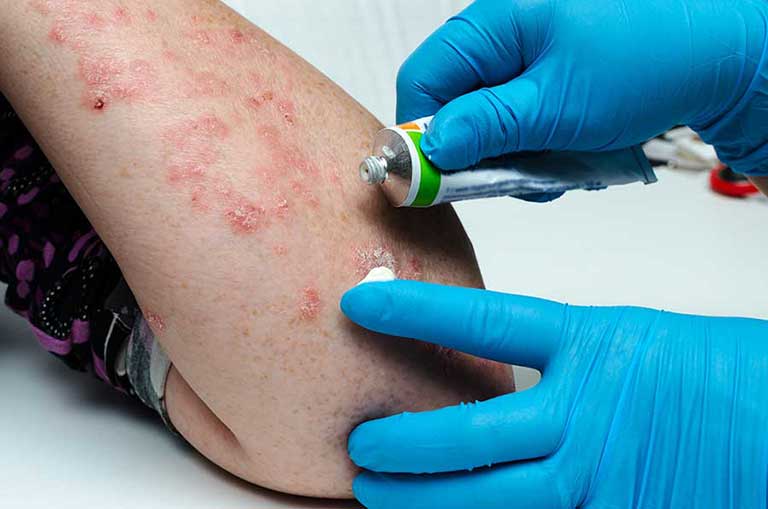
Psoriasis is a chronic disease that usually requires lifelong treatment. As the cause of the psoriasis is still unknown, treatment available is only for controlling sing and symptoms of the disease. There are different treatment options for psoriasis, such as topical treatments (applied externally to the skin), phototherapy (with UV light) or systemic medications.
References
- Feldman, S.R. Psoriasis: Epidemiology, clinical manifestations, and diagnosis. UpToDate [Internet]. 2020 [Cited 2020 Jan 31]. Available at: https://www.uptodate.com/contents/psoriasis-epidemiology-clinical-manifestations-and-diagnosis
- Feldman, S.R. Treatment of psoriasis in adults. UpToDate [Internet]. 2020 [Cited 2020 Feb 13]. Available at: https://www.uptodate.com/contents/treatment-of-psoriasis-in-adults
- Kang, S., Amagai, M., Bruckner, A.L., Enk, A.H., Margolis, D.J., McMichael, A.J., Orringer, J.S. Fitzpatrick’s Dermatology. McGraw Hill. 9th. ed. Buenos Aires, Argentina: Editorial Médica Panamericana S.A.; 2009. 720 p.
- World Health Organization (WHO). Global report on psoriasis [Internet]. 2016. Available at: https://apps.who.int/iris/handle/10665/204417
- Global Psoriasis Atlas (GPA). Key messages [Internet]. 2020. Available at: https://globalpsoriasisatlas.org/key-messages
- National Psoriasis Foundation (NPF). About psoriasis [Internet]. 2020 Mar 8. Available at: https://www.psoriasis.org/about-psoriasis
- National Psoriasis Foundation (NPF). Gluten-Free Diet [Internet]. 2019. Available at: https://www.psoriasis.org/treating-psoriasis/complementary-and-alternative/diet-and-nutrition/gluten-free-diet
- Barrea, L., Nappi, F., Di Somma, C., Savanelli, M.C., Falco, A., Balato, A., et al. Environmental Risk Factors in Psoriasis: The Point of View of the Nutritionist. Int J Environ Res Public Health [Internet]. 2016 Jul;13(7):743. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4962284/. doi: 10.3390/ijerph13070743
- European Academy of Dermatology and Venereology (EADV). Psoriasis can be hereditary [Internet]. 2019. Available at: https://www.eadv.org/cms-admin/showfile/9635-EADV%20PSORIASIS-7-Psoriasis%20and%20genetics.pdf
- Gudjonsson, J.E., Elder, J.T. Chapter 28: Psoriasis [Internet]. 2019. Available at: https://accessmedicine.mhmedical.com/content.aspx?sectionid=210417798&bookid=2570&R esultclick=2
Frequently asked questions about psoriasis
Psoriasis affects more than 60 million people worldwide.
It affects men and women equally and occurs more commonly in adults than in children. Psoriasis can occur at any age. While some studies indicated the average age of onset for psoriasis was 33 years of age, and 75% of cases occurred before 46 years of age (93), others suggested that the onset of psoriasis was bimodal with two peaks of the disease – the first between 16 and 22 and the second between 57 and 60 years of age.
Psoriasis has a hereditary component. That is, if you have psoriasis, your child is more likely to have it than other people. However, there are other factors that also play a role. The most important risk factors for psoriasis are obesity, smoking, alcohol use, infections, stress and some drugs.
No, psoriasis is not contagious, neither by contact nor by any other transmission mode.
Psoriasis cannot be cured. At present, there is no treatment that cures psoriasis. However, there are many medications that control the symptoms and allow you to lead a normal life.
Most people have mild psoriasis that is controlled with certain measures (such as hydrating the skin daily) and topical medications.
However, in some people, the disease affects a larger skin area or the joints or has a significant impact on the sufferer’s well-being and quality of life. In these cases, psoriasis may require other medications, either in tablets or in an injected form. Adequate and effective treatments are available for each person and for each type of psoriasis.
Psoriasis is a visible disease and because of that it can affect your quality of life. However, it does not impact all the people in the same way. It depends on many factors, such as the extension and intensity of the disease, the social environment and the personality of the sufferer. Anxiety and depression are frequent. To improve your quality of life, it is important for you to follow the treatment prescribed by your doctor, to maximize remission times and reduce the risk of other psoriasis-related diseases.
It is not known. It is impossible to predict how psoriasis will evolve in a specific person, or how long the flare-ups and remissions will last.
The doctor will adjust treatment based on disease course.
To date, diet has not been shown to be a risk factor to develop psoriasis. Therefore, there is no known food that causes psoriasis. Moreover, there is no scientific evidence to support a "diet for psoriasis".
However, it should not be forgotten that obesity is in fact a risk factor for psoriasis. Hence, following a hypocaloric or low-calorie diet to lose weight is beneficial for overweight people. In addition, psoriasis can be associated with cardiovascular diseases, and, therefore, a healthy, balanced and beneficial diet for the heart, such as a Mediterranean diet, is highly recommended.
Furthermore, if you have psoriasis and celiac disease, eliminating gluten from your diet can improve psoriasis, according to the National Psoriasis Foundation, which, on the other hand, does not recommend this type of diet in people without gluten intolerance.

