All about Atopic dermatitis
Atopic dermatitis (AD), or atopic eczema, is a non-contagious chronic, inflammatory disease of the skin.

Diagnosis
The diagnosis of AD is apparently easy, although unfortunately there is not a specific diagnostic laboratory marker test available. In most cases, therefore, clinical signs will be used for the diagnosis. This will be conducted based on the patient's medical history, specific clinical symptoms and the exclusion of other non-inflammatory skin disorders. The most distinctive and constant characteristics of the disease are pruritus (itchy skin), family and personal history related with atopy (allergic diseases), and chronic skin lesions (almost always typical) occurring during an outbreak. Furthermore, patients may present skin dryness and other cutaneous lesions such as serous exudates (watery plasma), excoriation (skin abrasions) , papules (pimples) and lichenification (thickening and leathery skin). In the absence of pruritus, the diagnosis of AD should be doubted, and differential diagnoses should be performed to safely determine the patient's illness.
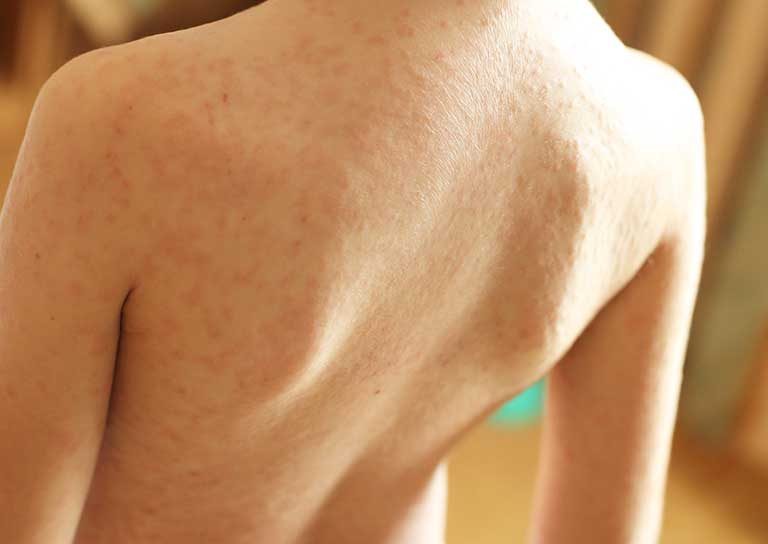
AD should be differentiated from other red, scaly skin conditions. It is often difficult to separate AD from seborrheic dermatitis in infancy, and the two conditions may overlap in this age group. Particularly if not responding to therapy, the diagnosis of AD should be rereviewed and other disorders considered, including more serious nutritional, metabolic, and immunologic conditions.
Eighty percent of patients with AD may present with high serum levels of Immunoglobulin E (IgE) antibodies. However, this information is clinically and prognostically insignificant since IgE is usually high in patients that also present with clinical respiratory allergy or food allergy.
In some patients, a skin biopsy may be necessary to rule out other conditions; however, histopathological findings only serve to reflect the stage of the eczema (acute, subacute or chronic); they are not specific to AD, so they cannot be used as a diagnostic test.
Microbiological cultures for the detection of fungi, bacteria and viruses may serve to rule out infectious pathologies similar to AD, such as tinea, impetigo, etc.; or to detect secondary infections that complicate the lesions of the atopic eczema.
References
Eichenfield, L.F., Tom, W.L., Berger, T.G., Krol, A., Paller, A.S., Schwarzenberger, K., et al. Guidelines of care for the management of atopic dermatitis: section 2. Management and treatment of atopic dermatitis with topical therapies. J Am Acad Dermatol. 2014;71(1):116–32.

